Scientists have discovered the precise amount of sleep needed to help fend off chronic illness, according to a new study published in BJM Open Diabetes Research Care.
So, if you are among the many people who wake up during the night, or if you are one of the millions already living with diabetes, sleep could be your best ally. But not just any amount. Researchers found that the optimal duration for reducing the risk of developing type 2 diabetes is approximately seven hours, 19 minutes, and 12 seconds.
The study analysed 23,475 Americans, comparing their sleep patterns with their estimated glucose disposal rate (eGDR), a widely used indicator of insulin resistance. The higher the eGDR, the lower the risk of insulin resistance, a condition that often precedes type 2 diabetes.
Diabetes remains a major global health challenge. According to the CDC, more than 40 million people live with diabetes in the United States, while the UK counts about 5.8 million cases. Across Europe, it is estimated that more than 60 million adults have diabetes, and this figure has steadily increased over the past generation as populations age and lifestyles change.
Diabetes occurs when the body either does not produce enough insulin or cannot use it properly, causing blood glucose, or sugar, levels to become too high.
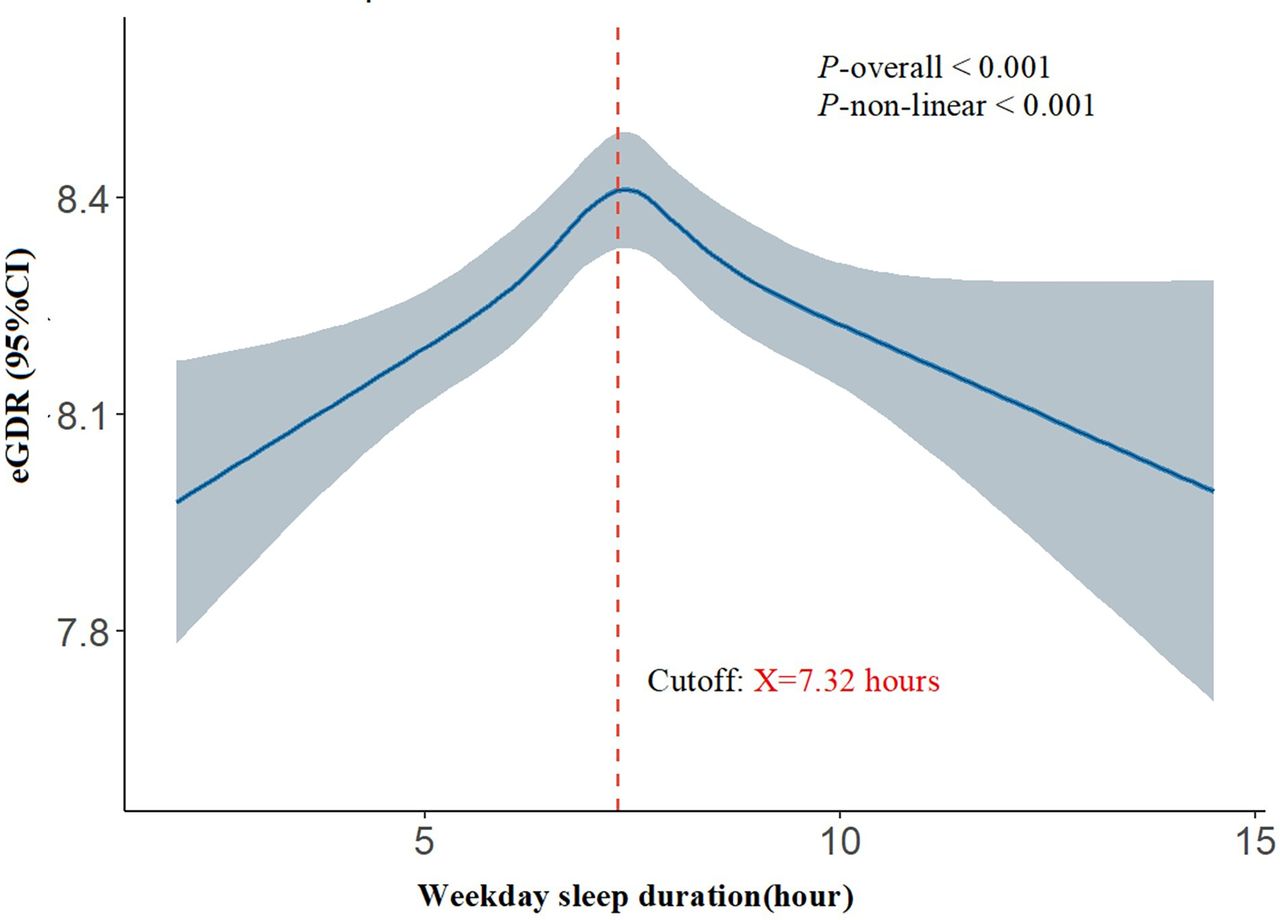
One of the most interesting findings is that both too little and too much sleep appear to affect insulin resistance. Researchers have observed an inverted U-shaped relationship between sleep duration and metabolic health. Up to around 7.3 hours, getting more sleep improves insulin sensitivity. However, beyond this point, additional sleep appeared to worsen it.
Thinking of opting for a weekend lie-in to compensate for a week of poor sleep may not help either, unless certain conditions are met. After analysing different sleep patterns, scientists concluded that extra sleep is only beneficial in moderation, primarily for those who accumulate sleep debt during the week. For those who already sleep enough, however, it may actually be detrimental.
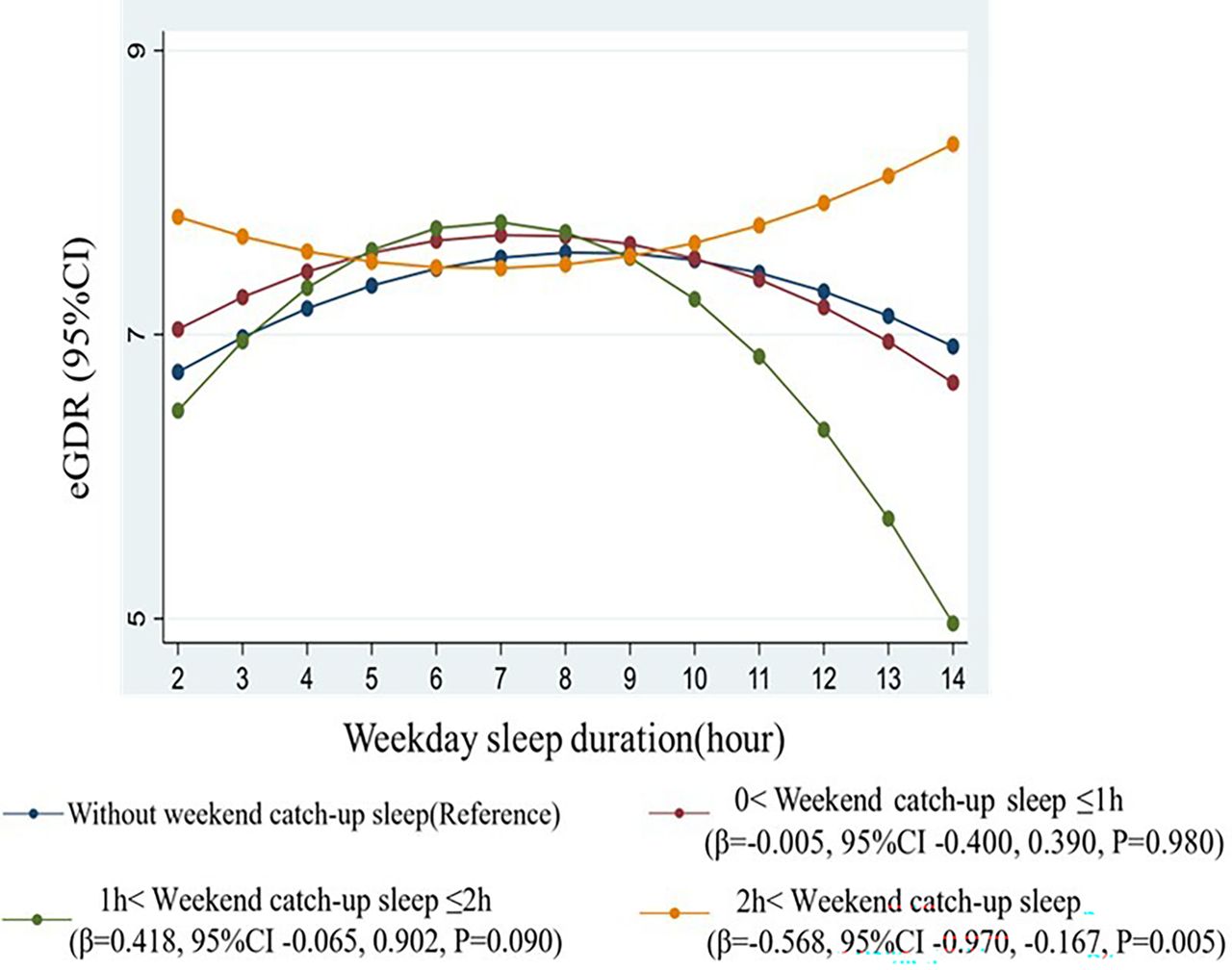
One study from 2024 did find that catching up on sleep reduced the risk of stroke or heart attack by around 19%. Nevertheless, the relationship between sleep and metabolic health remains complex.
This is where the real difficulty lies. Improving sleep is often easier said than done. The authors describe this as a “potential vicious cycle”: metabolic dysfunction disrupts normal sleep patterns, and high blood sugar can trigger the “dawn phenomenon” or frequent nighttime urination. Abnormal sleep, in turn, further aggravates metabolic health.
Naveed Sattar, a professor of cardiometabolic medicine at the University of Glasgow, told The Independent that poor sleep often leads to poorer appetite control, meaning people “tend to eat more and be less careful in choosing what they eat.”
The team cautioned that their research is observational and cross-sectional and cannot prove direct cause and effect. However, they suggest that sleep patterns, particularly attempts to compensate for sleep loss at the weekend, could become an important consideration for healthcare professionals managing diabetes risk.
But how does one actually achieve the right amount of sleep?
Although advice is abundant, ranging from 8-6-4 breathing and herbal infusions to melatonin and strict “no-screen” rules, real life rarely follows perfect sleep hygiene.
The next breakthrough may not lie in another study, but in technology: a personalised app that combines real-time glucose monitoring with precision sleep tracking and sleep-inducing sounds. Such apps may already exist, or be closer than we think.













